MYASTHENIA GRAVIS:
Myasthenia gravis has been considered a rare disease; however, the adult-onset form
seems to be on the rise. Whether this represents improvements in diagnostic criteria and
methodology or a real increase in the condition remains unsure. On the other hand, this may
represent an increase, similar to that for other immune-related diseases.
It has been reported in
young dogs (juvenile form) and adult dogs and cats.
The juvenile form represents a genetic
problem where there are too few acetylcholine receptors at the neuromuscular junction.
The
adult form represents an auto-immune disease where there is the production of antibodies against
the acetylcholine receptor, demonstrated by elevations in circulating anti-receptor antibodies.
With either the juvenile form or the adult form, myasthenia represent a functional deficiency of
sustainable release of acetylcholine from the pre-synaptic neuron at the neuromuscular junction.
This distinguishes myasthenia from the myasthenic-like disease of OP intoxication.
The disease can be seen in any adult dog or cat, the young adult German Shepherd dog
being overly represented.
There may be an inciting febrile episode, but often no inciting cause is
found. Animals present with weakness and exercise intolerance. There may be changes in bark,
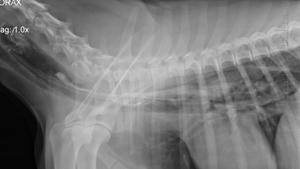
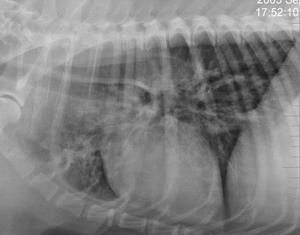
difficulty in swallowing and prehending food. Regurgitation and megaesophagus may be present.
Some cases present in a myasthenic crises where the animal has collapsed and is unable to rise.
At this time, there may be muscle flaccidity.
In uncomplicated myasthenia gravis (those without pulmonary pathology from aspiration
pneumonia), the animal demonstrates progressive weakness on movement which improves with rest. Mild cases may be difficult to differentiate from animals with polymyositis.
Except when in
a myasthenic crisis, neurologic assessment is usually normal.
The diagnosis is suspected by
demonstration of a normal needle EMG, normal nerve conduction velocities and decremental
response to repetitive nerve stimulation. (We normally stimulate at 10/second, recording the first
9 stimulations. An abnormal response is when the 4th and 9th waves are <85% of the initial
wave)
Confirmation of the diagnosis is made by demonstrating elevated serum anti-acetylcholine
receptor antibodies (>0.06 ng/ml).
Additional confirmation can be made by positive response to
edrophonium HCl either in the conscious animal or during the EMG procedure. (Remember the
OP intoxication can look like myasthenia. I, therefore, do not give edrophonium until I have
checked serum cholinesterase levels.)
The treatment of myasthenia is to suppress the production of antibodies and to increase
acetylcholinergic function. The former is usually done by the administration of prednisolone at
1-2 mg/kg/day. The dose is reduced while monitoring the serum anti-receptor antibody levels.
The latter is done by giving pyridostigmine at 10-60 mg twice a day (depending upon the size of
the patient). During a myasthenic crisis, intramuscular injections of neostigmine (0.5-2.5 mg)
may be given in cats and dogs.
The prognosis is guarded. In uncomplicated cases, the signs may
resolve and go into remission. In cases with aspiration pneumonia, the prognosis is usually poor.
Recently, immunotherapy has offered new hope in treating refractory cases. By inoculation of
patients with purified anti-receptor antibodies, they produce anti-idiotypic antibodies which can
help control their altered immunity. Since this may be a disorder which is developed in response
to environmental intoxication with resultant failure of the healing process, dietary
supplementation and antioxidant support may help prevent this disease.
volver a la pûÀgina principal de polineuropatûÙas
|




 miles de casos clûÙnicos
miles de casos clûÙnicos